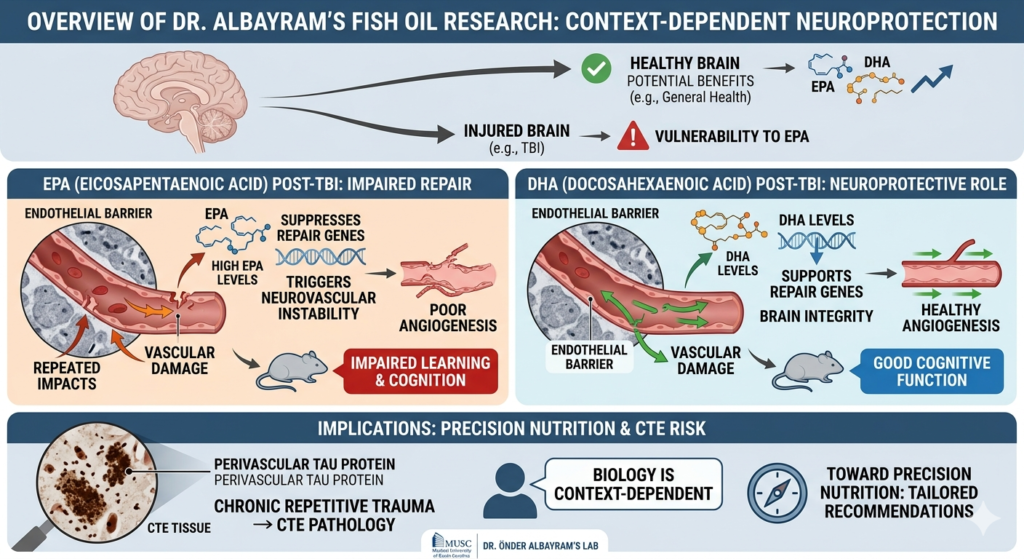
Research led by Dr. Önder Albayram, an Associate Professor at the Medical University of South Carolina (MUSC), has recently challenged long-standing assumptions regarding the universal benefits of fish oil for brain health. His findings highlight a “context-dependent metabolic vulnerability,” specifically in the context of traumatic brain injury (TBI) and recovery.
The Core Finding: EPA and the Post-Injury Brain
While omega-3 fatty acids are generally regarded as neuroprotective, Dr. Albayram’s research, published in Cell Reports in March 2026, suggests that a specific component—eicosapentaenoic acid (EPA)—may paradoxically hinder the brain’s ability to repair itself after repeated mild head injuries (Karakaya et al., 2026).
- Mechanism of Impairment: The study found that elevated EPA levels in a sensitive brain state (such as following TBI) trigger neurovascular instability. This instability disrupts the formation of new blood vessels (angiogenesis) and weakens the endothelial barrier, which is essential for transporting nutrients and oxygen to damaged tissue (Karakaya et al., 2026).
- Long-Term Consequences: In mouse models, long-term fish oil supplementation following repeated impacts was linked to poorer spatial learning and neurological performance over time. This was accompanied by a significant accumulation of perivascular tau protein, a primary marker of Chronic Traumatic Encephalopathy (CTE) (Karakaya et al., 2026).
Key Distinctions: EPA vs. DHA
A critical aspect of Albayram’s work is the distinction between the two primary types of omega-3s found in fish oil:
- DHA (Docosahexaenoic Acid): Dr. Albayram notes that there remains strong evidence for the benefits of DHA, which serves as a major structural component of neuronal membranes and generally supports brain integrity.
- EPA (Eicosapentaenoic Acid): This component was identified as the driver of metabolic reprogramming. Under “permissive metabolic conditions” caused by injury, EPA suppresses the gene programs required for vascular repair and extracellular matrix organization (Karakaya et al., 2026).
Translational Relevance to CTE
The research team corroborated their animal findings by analyzing postmortem human brain tissue from confirmed CTE cases.
- The human samples showed a “convergent signature” of disrupted fatty acid balance, with significantly higher levels of EPA and DHA compared to control groups (Karakaya et al., 2026).
- This suggests that the metabolic shifts observed in the lab are mirrored in humans with histories of repetitive head trauma, potentially linking chronic supplement use in athletes or military personnel to an accelerated neurodegenerative path.
Scientific Context and “Precision Nutrition”
Dr. Albayram emphasizes that his research is not a call for the general public to stop taking fish oil. Instead, it serves as a warning that biological responses are context-dependent.
- Healthy vs. Injured Brains: For a healthy adult, fish oil may continue to provide cardiovascular and anti-inflammatory benefits.
- The “One-Size-Fits-All” Myth: The study argues for “precision nutrition,” suggesting that dietary recommendations must account for an individual’s specific neurological history and metabolic state.
References
Karakaya, E., Berber, B., Eskiocak, O., Edwards, J., Barker, R. B., Jamil, S., Li, W., Abdul, Y., Ericsson, M., Stein, T., McKee, A., Ergul, A., Beyaz, S., & Albayram, O. (2026). Eicosapentaenoic acid reprograms cerebrovascular metabolism and impairs repair after brain injury, with relevance to chronic traumatic encephalopathy. Cell Reports, 45(3), 117135. https://doi.org/10.1016/j.celrep.2026.117135
Did you have a specific interest in how these findings might impact sports medicine or general dietary guidelines?